Leg Pain and Weakness? – Do You Have Radiculopathy?
Leg pain and/or weakness are common complaints, and often some of the most enigmatic symptoms for doctors to diagnose and treat. Although leg pain can be the result of a variety of causes, one of the most common reasons it develops is a condition known as radiculopathy. Radiculopathy is caused by one or more of the spinal nerve roots being pinched. In the case of leg pain or weakness, the compression of low back nerve roots is usually the culprit. Before we discuss the implications of nerve pinching in the back, it is important to note that back pain is often NOT present at all, even if the leg symptoms are severe. Radiculopathy patients with leg pain and weakness, who are not experiencing back pain, often go from doctor to doctor seeking answers. They usually end up with a prescription for drugs that only mask the symptoms. Unfortunately, the condition worsens over time.
The most common cause of radiculopathy, with or without back pain, is the result of degenerative changes in the spine. As the disc and other structures in the spine degenerate from age and wear, nerves gradually start to get pinched. The symptoms can creep up on people so gradually that they simply chalk them up to aging. Sometimes the symptoms may start as a simple numbness or tingling. Occasionally, patients say they stumble when they walk, or their knees go weak and buckle for no apparent reason. Their legs may feel “heavy.” Burning and aching in the legs and feet are not uncommon.
Radiculopathy and Diabetic Neuropathy Can Produce Some of the Same Symptoms…Make Sure You Are Not Misdiagnosed.
 If a person is diabetic, doctors will usually blame neuropathy-like symptoms on the diabetes. We frequently see patients who were misdiagnosed with diabetic neuropathy, who instead were experiencing lumbar radiculopathy. The reason for doctors missing the diagnosis is often because the patient wasn’t experiencing back pain. Sadly, the patient is prescribed Gabapentin, or Lyrica, when the problem could have been corrected without drugs. Diabetes can sometimes cause these symptoms, but radiculopathy should also be considered as a possibility because it can cause similar symptoms. If the patient is experiencing leg symptoms and back pain simultaneously, most doctors will have enough clues to connect the dots and realize that the leg symptoms are emanating from the low back. It takes more “detective work” to accurately diagnose a patient with radiculopathy, if they are not also experiencing back pain.
If a person is diabetic, doctors will usually blame neuropathy-like symptoms on the diabetes. We frequently see patients who were misdiagnosed with diabetic neuropathy, who instead were experiencing lumbar radiculopathy. The reason for doctors missing the diagnosis is often because the patient wasn’t experiencing back pain. Sadly, the patient is prescribed Gabapentin, or Lyrica, when the problem could have been corrected without drugs. Diabetes can sometimes cause these symptoms, but radiculopathy should also be considered as a possibility because it can cause similar symptoms. If the patient is experiencing leg symptoms and back pain simultaneously, most doctors will have enough clues to connect the dots and realize that the leg symptoms are emanating from the low back. It takes more “detective work” to accurately diagnose a patient with radiculopathy, if they are not also experiencing back pain.
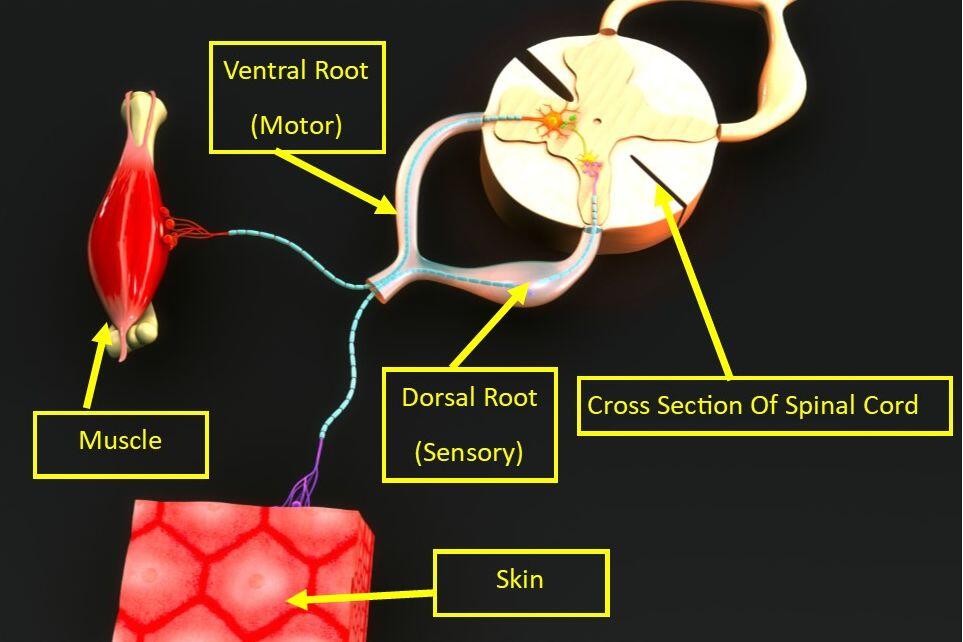
Since radiculopathy can result from compression of a nerve root where it exits from the spine, it is important to know exactly what’s happening when it gets pinched. There are 31 pairs of spinal nerve roots, and each contains two branches called a dorsal root and ventral root. The ventral root provides motor impulses to muscles so they can contract and move joints. The dorsal root provides sensory impulses that travel from patches of skin called dermatomes back to the spinal cord and brain. The dorsal roots allow you to feel the sense of touch on the skin surface. The nerves also transmit other sensory stimuli, such as the sense of hot, cold, vibration, and light touch.
 In most cases, the dorsal root will be pinched first, causing pain, numbness, tingling, and/or burning to travel down the dermatome. A doctor can identify which area of the spine the nerve is being pinched by which dermatome, or patch of skin is being affected.
In most cases, the dorsal root will be pinched first, causing pain, numbness, tingling, and/or burning to travel down the dermatome. A doctor can identify which area of the spine the nerve is being pinched by which dermatome, or patch of skin is being affected.
Eventually, the ventral root gets pinched and causes weakness to the respective muscle it innervates. The weakness in the muscle occurs because the motor impulses are being choked off by the nerve pinch.
As the dorsal root gets pinched with more pressure, the pain, numbness, tingling, or burning gets worse. Likewise, as the ventral nerve root is subjected to more compression, the respective muscle it supplies gets weaker. Eventually, the muscle may weaken to the point that it begins to shrivel up, or atrophy. If the ventral root gets pinched by itself, with no dorsal root compression, the only symptom will be muscle weakness. In this scenario there would not be any pain at all. So, weakness is as important of a symptom as pain. It can also indicate the potential for nerve damage.
Radiculopathy Can Occur at Any Level of the Spine
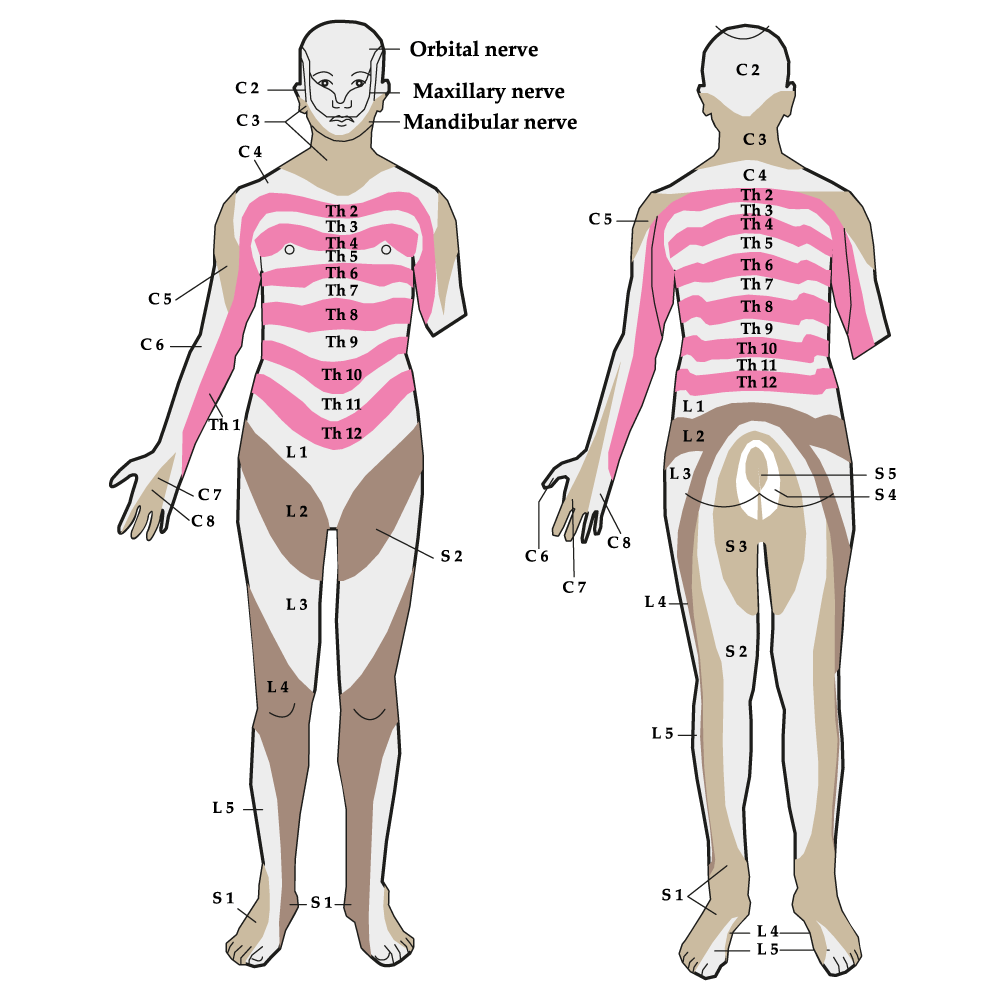
Nerve compression that leads to radiculopathy can occur at any level of the spine. The low back and neck are the two most common locations. However, it can also occur in the Thoracic Spine and cause any of the symptoms listed above. The pain symptoms associated with radiculopathy in the Thoracic Spine are called intercostal neuralgia. In this case, the symptoms can radiate around the rib cage. We have seen patients with intercostal neuralgia who thought they were having heart problems because the pain was referring across their chest at the level of the heart. The dermatome chart on this page shows the nerve levels that go across the chest area.
Cervical radiculopathy can cause pain, numbness, tingling, burning, and/or weakness in the shoulders, arms, hands or fingers. The radiculopathy arm, hand, and finger symptoms are to the neck, what the thigh, leg, foot, and toe symptoms are to the low back. The dermatome chart on this page also illustrates the cervical levels that affect the different patches of skin in the upper extremities.
What Can You Do For Radiculopathy?
At Health 1st Wellness & Physical Medicine we utilize a number of treatment modalities that help radiculopathy, one of which is called Spinal Decompression. The most common causes of radiculopathy can include disc bulges, disc degeneration, facet joint hypertrophy, foraminal narrowing, and more. We utilize MRIs to determine if patients are candidates for treatment, and also use them to enhance treatment precision. The treatment is drugless and non-surgical. If you or someone you know has symptoms related to radiculopathy and you don’t want injections, or back surgery, Spinal Decompression Therapy provides a highly effective and conservative alternative. We have provided thousands of successful treatments. Call our office today to find out more.
-Dr. Randall Roth
